You never realize how much your feet impact your life and your wellbeing until something goes wrong. For many people, plantar fasciitis is a constant reminder of how important foot health can be. Sadly, for many, the diagnosis of plantar fasciitis means a lifelong uphill battle against its symptoms because there is currently no cure. However, with time, patience, and due diligence, you can manage your plantar fasciitis symptoms and live life to its fullest.
What Is Plantar Fasciitis?
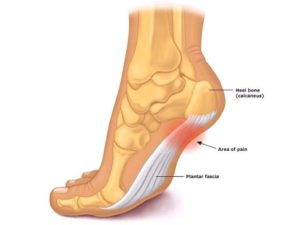
It is easiest to remember what a word or diagnosis is if you break it down into parts. The suffix –itis is used for inflammation. This means that plantar fasciitis is an inflammation of the plantar fascia (*sometimes, we’ll get to how this can be a misnomer in a minute). Plantar means that this anatomical structure is located on the bottom of your foot and fascia is typically a band of tissue. Putting it all together, plantar fasciitis is the inflammation of the tissue band on the bottom of your foot.
See also: medical cannabis doctor
Your plantar fascia starts at your heel and runs to your toes. It is mainly responsible for the arch of your foot. So why do you even have this bizarre arch? Well, your foot takes a lot of impact. It takes the initial blow of pressure every time you stand, walk, run, jump, or basically do any moving. The arch of your foot acts as a shock absorber. It helps to dissipate the pressure that is constantly being put on your feet. This is why your plantar fascia is so critical to everything you do. In the same vain, it is also why this condition can be so debilitating.
What Causes It?
So we now know that every time you are on your feet, your plantar fascia at the bottom of your foot is working to distribute the pressure on your feet. It is easy to understand then, what can cause inflammation of this tissue to occur. Long-distance running is a common culprit[5]. Think of how much pressure is being put on the plantar fascia for long periods of time. Obesity is another common risk factor because there is extra pressure on the foot with each step. You can also develop plantar fasciitis by wearing the wrong shoes. High heels are a major offender, but even wearing the wrong arch support for your feet could result in damage to your plantar fascia. Some people are more susceptible than others, so not all long-distance runners or people who are overweight will have plantar fasciitis (although chronically wearing bad shoes almost guarantees it). But if you are one of the many who have to battle it, you may be wondering exactly what is going on down there.
Well, every time there is excessive pressure being put on the plantar fascia, microscopic tears form. These microscopic tears can cause inflammation which worsens the symptoms, but the tears themselves are enough to force you off of your feet. So just because you have plantar fasciitis, doesn’t mean you actually have inflammation although it is common. However, it may change the way you manage some of your symptoms.
How Do I Know If I Have It?
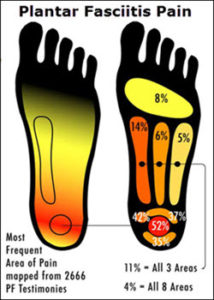
Plantar fasciitis will be diagnosed by your doctor because other conditions will need to be ruled out to assure that you do have plantar fasciitis and not something else. But what should you be on the lookout for? Many people with plantar fasciitis have heel pain that is at its worst in the morning but will lessen throughout the day (do not be fooled and still go to see your doctor). You may also notice that the bottom of your foot is tender to the touch or it may be a bit swollen and red. You’ll also want to observe the arches of your feet. Are they abnormally high or low? Do they feel tight to the touch? If you are noticing that you fit any of these symptoms, schedule an appointment with your doctor.
What to Expect
The Visit to the Doctor
There is no need to panic when you’re going to head to the doctors. There is a surgical procedure to help with plantar fasciitis, but most people are fine with conservative treatments they can do at home (so go ahead and breathe).
The first thing your doctor will do after your history and physical (make sure to tell them if you wear crazy shoes every day or run a lot) is perform a physical exam of your foot. It is not invasive and should not be overly painful, but your foot will be touched. Next, your doctor might order x-rays to rule out other conditions like a fracture. Many foot disorders present the same way, but the treatment is different. This is why you want to get a diagnosis before jumping into treatments. For example, some people with plantar fasciitis like to stretch their arch by stepping on a tennis ball while seated. This would cause unreal pain to you and unnecessary injury to a bone fracture if you self-diagnosed yourself incorrectly.
Professional Treatments
There are a few treatment options that your doctor can offer to you, outside of the things you can do at home (we’ll talk about those in a moment). First, they can make you a boot cast that you will wear for about 6 weeks. This boot is designed to help keep your plantar fascia stretched. Think about the strings on a bow, the more taught and tight they are the easier it would be to snap them. If the strings on the bow are long and loose it is harder to damage them. This same principle applies to your plantar fascia.
An alternative to the boot is a night splint. This is essentially a splint you will wear on your foot while you sleep. The splint will stretch out your plantar fascia for you, making it looser and less susceptible to damage. Of course, many people have difficulty sleeping with it on because it can get uncomfortable. One of the reasons your plantar fasciitis is at its worse in the morning is because it tightens up at night. This microscopic tears want to heal. Just like your muscles, your plantar fascia wants to heal in a contracted position because that is the most efficient way to heal (think of having to build a bridge that is 1 foot long as opposed to 5 feet). Again, it works well but it can be a pain. This is why many people opt for the boot even though it is inconvenient. However, for those that can tolerate the night splint, it’s a more socially acceptable alternative.
Another option is a shoe orthotic (insert). Some are designed to stretch your plantar fascia like the boot, but most are made to work with what you have. So let’s think about your feet. If putting pressure on your arch (flattening it out) causes damage, then putting something in your shoe that keeps your foot from flattening will keep it from being injured. The main objection to this treatment is obviously the aesthetics. If you developed plantar fasciitis by wearing high heels you may be less than thrilled to wear the wide, clunky shoes that can hold an orthotic.
Your doctor may also offer to give you steroid shots in your foot. This helps if you have inflammation. However, some people experience tenderness where the shot occurred, which sort of defeats the purpose. But it should give you about a week of relief so this option may work for you.
For plantar fasciitis that does not respond to home treatments or professional treatments, you may need to consider surgery. The surgery will be performed by an orthopedic surgeon who will cut part of the plantar fascia. Going back to our analogy of the bow strings, having a thick band of strings will have more tension than a few strings. This is what the surgery does to your plantar fascia. It relieves some of the pressure, ultimately lessening the amount of micro tears that can occur. Of course, healing time is a consideration.
As a less invasive option, your doctor may also prescribe you acetaminophen or ibuprofen (also known as Advil or Tylenol). You may be taking these chronically for the rest of your life so don’t start taking them on your own. Get your doctor’s permission first to ensure your safety. The good news is that this may be an easy and quick treatment that provides you with the temporary relief you need to live your life each day.

Home Treatments
Before giving you professional treatments, your doctor will probably first opt for home treatments to see if they are enough to alleviate your symptoms. For most people they are. It’s important to keep an open mind but also to be realistic with yourself. You will most likely have to perform your plantar fasciitis routine every day. Most people, though, are willing to take the time out to treat their symptoms because they can’t continue on with their day if they don’t. This is also important to think about. It may be worth doing an extra 15 minutes of exercises in the morning if it means you aren’t confined to a seated position for the rest of the day. So what are your options?
First, your doctor may suggest resting for a few days while applying ice to your feet at the beginning and the end of the day to reduce swelling and inflammation. These are by no means cures, but they can get you back to a good starting point. Obviously, resting all the time is not feasible, so after your initial period of rest you’ll want to find other ways to manage.
If you like the ice, you can continue to use it as a method of treatment. Wrap your ice in a towel and don’t leave it on for more than 20 minutes a day otherwise you can cause injury. Also, if you have decreased sensation in your feet (especially if you are diabetic), reconsider the ice. You may be causing damage that you can’t feel which would only make your situation worse. There are plenty of other options anyway.
One of my favorite options is stretching. This is because it helps with the range of motion of your joints while also alleviating your symptoms- talk about a win-win. Stretches of your plantar fascia and Achilles tendon are most often recommended (the Achilles tendon attaches to your heel too so if affects your plantar fascia). So how do you stretch them?
If you are flexible enough, you can sit and cross an ankle over your knee. Now that your foot is easily accessible, grab your toes. Gently stretch them backward. Next, place your hand on the ball of your foot and also gently stretch backward. Hold each stretch for at least one minute to thoroughly lengthen your plantar fascia. If you are not flexible enough, remain seated and strategically place a tennis ball under your toes and then the ball of your foot to perform the same stretch.
To stretch your Achilles tendon, you can stand or sit facing a well. Place the ball of our foot on the wall while your heel remains on the floor. Hold this stretch for at least one minute. It’s that easy!
Do Not Wait!
Don’t wait to see if your foot pain subsides on its own. See a doctor and get a diagnosis as soon as possible so that you may begin treatment. If you wait to address your plantar fasciitis, it can quickly spread into a body-wide problem. This is because the foot pain caused by plantar fasciitis will change the way you walk. This means that you will begin to improperly use your ankles, knees, and hips, which will then also impact your back. Suddenly, a problem that started in your feet has taken over your entire body. Don’t let it happen.
Even if you manage to avoid hurting all of the joints in the lower half of your body, you are still at risk. Any pain that is not treated properly can lead to a chronic pain syndrome. This is because, by having pain for a long period of time, you are training your nerves to constantly feel pain. This might not turn off when the physical cause of pain is gone. This is a major problem for your wellbeing. If you can avoid it from occurring, then make sure you do!
More to read: Toenail Fungus – All You Need To Know

